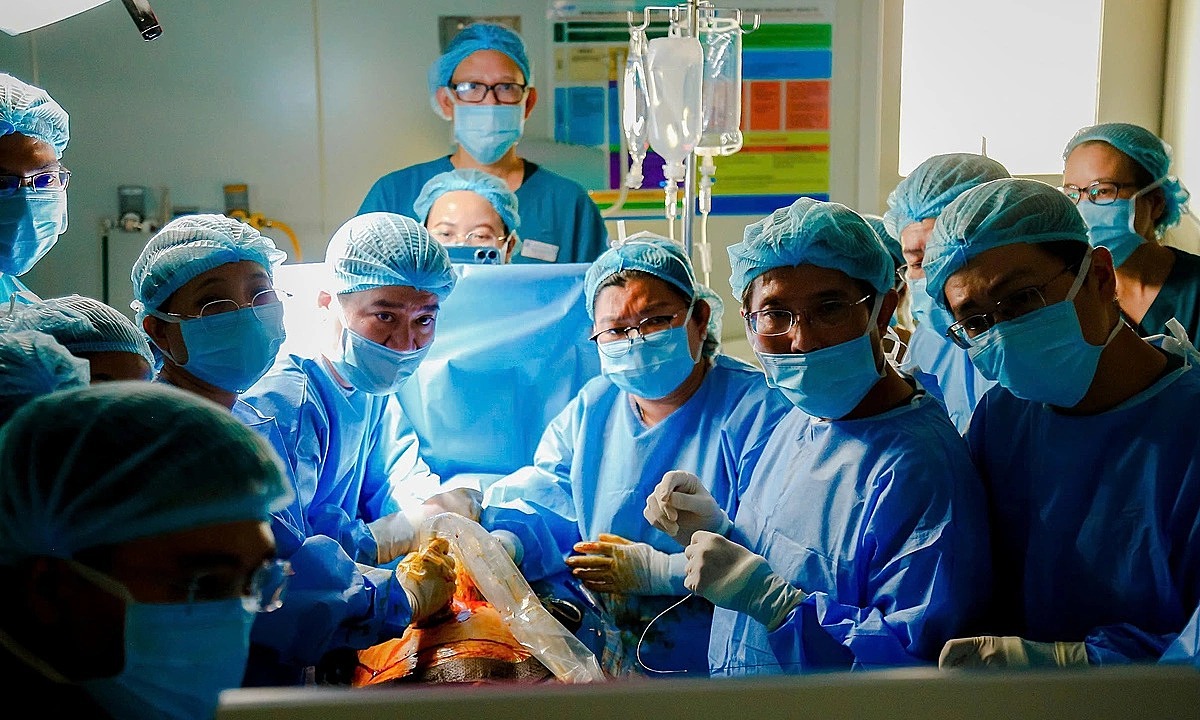
A 41-year-old Singaporean woman has given birth to a healthy baby girl after undergoing a rare, high-risk fetal heart surgery in Vietnam, marking a significant medical breakthrough that doctors say “rewrote the child’s fate.”
According to Tran Ngoc Hai, director of Tu Du Hospital in Ho Chi Minh City, the baby weighed 3.7 kg at birth, had a rosy complexion, breathed naturally without respiratory support, and is feeding and developing normally. She was born on July 19 in Singapore and later underwent a minor procedure to tie off two pulmonary arteries.
Just months earlier, when the fetus was 25 weeks old and weighed only 600 grams, doctors discovered a severe aortic valve stenosis: the main heart valve was almost completely sealed, and the left ventricle had shrunk to just 1.4 millimeters, the size of a pencil tip. A Vietnamese medical team used an ultra-fine needle to guide a catheter through the mother’s abdomen and into the baby’s heart, no larger than a strawberry, to repair the defect.
The intervention saved the baby’s life. Without it, doctors said, the condition would have been fatal after birth. Thanks to the early correction, the girl only needed a light follow-up procedure instead of major open-heart surgery.
The woman, who conceived through in-vitro fertilization after more than a decade of infertility, was referred to Vietnam by a Singaporean specialist in late May, a sign of growing trust in the country’s fetal medicine expertise. The case is now being reviewed by the Ministry of Health as Vietnam’s first documented fetal cardiac catheterization.
In June, the ministry honored doctors from Tu Du Hospital and Children’s Hospital 1 for their pioneering teamwork. Deputy health minister Tran Van Thuan called it proof of Vietnamese doctors’ determination to “push the limits of medicine” and a foundation for Vietnam’s emergence as a regional hub for fetal and personalized medicine.
At an international conference on Nov. 6, Hai described the case as part of a broader “revolution in fetal diagnostics.” Detecting heart and neurological defects before 13 weeks of pregnancy remains one of medicine’s toughest challenges, he said, but one that Vietnamese specialists are now embracing.
Key Details of the Medical Procedure
- Timing of Diagnosis:The condition was detected when the fetus was 25 weeks old.
- Weight at Diagnosis:The fetus weighed 600 grams.
- Medical Condition:Severe aortic valve stenosis, with the left ventricle shrinking to 1.4 millimeters.
- Procedure Used:An ultra-fine needle guided a catheter through the mother’s abdomen into the baby’s heart.
- Outcome:The surgery successfully repaired the defect, avoiding the need for major open-heart surgery.
Impact on the Patient
- Birth Weight:The baby weighed 3.7 kg at birth.
- Health Status:The baby had a rosy complexion, breathed naturally, and was feeding and developing normally.
- Follow-Up Procedure:A minor procedure was performed to tie off two pulmonary arteries.
Significance of the Case
- First Documented Case:This is Vietnam’s first recorded instance of fetal cardiac catheterization.
- Recognition:The Ministry of Health honored the medical teams involved in the procedure.
- International Attention:The case was discussed at an international conference, highlighting advancements in fetal diagnostics.
Future Implications
- Medical Advancements:The success of this procedure could pave the way for more complex fetal interventions.
- Regional Hub Potential:Vietnam is positioning itself as a center for fetal and personalized medicine.
- Global Collaboration:The case reflects growing trust in Vietnamese medical expertise, especially in the field of fetal medicine.
This remarkable case not only showcases the skill and dedication of the medical professionals involved but also highlights the potential for advanced fetal care to save lives and improve outcomes for newborns worldwide.